-

Accidental Botulism Poisoning: A Case of Pickled Herring
Garrett Spencer and Greg Flick
INTRODUCTION: Botulism is a rare cause of neuromuscular weakness that presents a diagnostic challenge in the face of respiratory collapse. Pupil and bulbar paralysis aid prompt recognition and treatment, as clinical confirmation can be time intensive and limited by sample integrity. Early treatment can halt paralysis and prevent ICU and ventilator days.
CASE DESCRIPTION: A 74-year-old male with hypertension and DVT presented with acute weakness and respiratory failure after three days of cough and diarrhea. Upon ICU admission for mechanical ventilation, we discovered sluggish pupils, mild ptosis, and proximal muscle weakness. Symptoms then progressed to unresponsive pupils, complete ptosis, and complete paralysis. While we suspected a neuromuscular cause, no single cause was identified despite extensive workup and neurology consultation. Our differential was narrowed after electromyogram (EMG) demonstrated a pre-synaptic defect, indicating either Lambert Eaton or Botulism as culprits. Empiric treatment with botulism anti-toxin resulted in clinical improvement of ptosis and proximal weakness. While ventilated, he wrote of recent pickeled herring ingestion, possibly left unrefrigerated for a week. He ultimately received tracheostomy and transfer to long-term assisted care, and at discharge stool and serum testing for botulism toxin was still pending. While state-run testing finally returned negative, his illness was ultimately attributed to accidental botulism poisoning.
DATA:
Differential and Workup
Myasthenia Gravis • CT Chest: no mediastinal/thymic mass (thymoma) • Acetylcholine Receptor Ab: negative • Striated Muscle and Titin Ab: negative Lambert Eaton • Pre-synaptic defect on EMG: low motor amplitudes that increased with sustained exercise • Voltage Gated Calcium Chanel Ab: negative • CT Chest: no nodules or masses (paraneoplastic SCLC in 50%) Demyelinating Polyneuropathy • LP: Glucose 76, protein 53, WBC 0, RBC 0, lymphocytes 67% • CSF: Ganglioside GM1 Ab negative Botulism • Stool: rejected, poor specimen quality • Serum: small sample size, Endopep-MS assay negative Central and Infectious • MRI brain and C-spine normal Infectious • Treponemal Ab negative • Lyme Ab negativeBotulism Key Features
Exam • Respiratory collapse • Proximal then distal paralysis, rapid progression • Preserved sensation, reflexes • Bulbar Paralysis with pupil involvement, nystagmus Workup • Botulism Neurotoxin (BoNT) of fluid, serum samples • Mouse Bioassay Treatment • Botulism equine anti-toxin, early administration can reduce ventilator and ICU daysRESULTS / DISCUSSION: Yearly US incidence of botulism is 100 cases, and early treatment with equine anti-toxin reduces mortality and ventilation time1. Timely diagnosis is challenging as respiratory collapse overshadows subtle pupil and bulbar paralysis unique to botulism2. Lab diagnosis with Endopep-MS assay is not FDA approved and can be falsely negative with small samples3 while verified sacrificial mouse bioassays are rarely used2. Early suspicion should prompt anti-toxin treatment and discussion with the CDC’s botulism consultation service, who will supply anti-toxin and provide assistance with workup in conjunction with state health laboratories.
-

Addressing The Social Determinants of Health in the Clinic Setting
Larissa Sharma and Man Tran
INTRODUCTION: It is estimated that clinical care accounts for only 20% of health, while behaviors, physical environment, and social and economic factors determine the rest. The social determinants of health include the basic life needs of housing, food, transport, along with other factors that include employment, education, drug and alcohol use, dental and eye care, etc. Insecurity in these socioeconomic factors are expressed in chronic medical illness, mental health problems, substance use, all leading to high healthcare utilization. Healthcare costs and utilization decrease when when these needs are provided for. In a survey of 6,000 Providence patients, 50% expressed a social determinant need. Providence subsidizes Community Resource Desks around Oregon, staffed with bi-lingual resource specialists from local social service organizations, designed to connect individuals in need of support with resources available in their community. A model for referral to a local Community Resource Desk was created and patients referred to the desk to provide for any social needs.
OUTCOMES: More than 250 of our Providence St Vincent Resident Clinic patients were referred and offered resources in the 1st year of the project. At peak screening 30-40 patients were referred monthly. Most of these patients would not have otherwise come to our attention. Most common resources provided: dental care, housing/rent, utilities, food, transport, employment assistance, health insurance, English/computer classes. We are better able to care for our most vulnerable patients including non- English speakers, uninsured, and Medicaid/Medicare patients. Clinic staff and providers expressed satisfaction with the simplicity of the process.
DISCUSSION: ● This system allows for more comprehensive care, streamlines workflow for providers, and allows providers to practice in a way more in line with their goals. In addition, multiple studies show cost savings benefits to implementing similar programs. ● One study with a similar intervention noted 10% yearly health care cost reduction for those who had their social needs met. ● Vermont Health system- implemented multidisciplinary team care model adding Community Health Specialist. Found tremendous cost benefits and decrease in hospital admission rates(declined 21%) and ED utilization(declined 31%). Per person per month costs fell 36%. ● We are in the process of collecting data on how this is impacting our quality metrics including healthcare utilization, hospitalization rates and per patient/per month costs.
-

Battling the Stigma: HIV Screening in Resident Primary Care Clinic
Garrett Spencer, Laura Loertscher, and Shelley Sanders
INTRODUCTION: HIV affects ~1.2 million in the US, with 25% unaware of their statusand annual incidence of 50,000. Early detection and treatment reduces risk of AIDS-related deaths and transmission. Both the CDC and the US Preventative Service Task Force recommend routine HIV screening. The Providence Medical Group at St Vincent (PMG-STV) resident clinic has no routine screening protocol. • 24% (757/3139) of all clinic patients have ever been screened. • Of active clinic patients seen quarterly, 5% are offered screening with only 3% completing screening. We implemented and measured a clinic-wide HIV screening protocol leveraging existing clinic workflows. We aimed to increase screening of active clinic patients from 3% to 25% at one year.
METHODS: Using a time-series design we measured quarterly rates of HIV screening tests ordered and resulted in active clinic patients, ages 18-65 and seen in office, during the study period. We utilized a pre-existing preventative healthcare workflow for routine cancer screening, influenza vaccines, etc. We introduced this workflow to residents and staff prior to our go-live date.
RESULTS / DISCUSSION: Our primary outcome was to increase quarterly HIV screening rate of active patients, with a secondary outcome to increase overall clinic HIV screening rate. We increased the quarterly screening rate of active patients from 3.34% to 9.19% (P
-
Catastrophic Antiphospholipid Syndrome
Gabriel Hocum and Jeff Youker
INTRODUCTION: Catastrophic Antiphospholipid Syndrome (CAPS) is a rare and extreme manifestation of Antiphospholipid Syndrome (APS) that features widespread thrombotic disease affecting multiple small vessels in a short time frame. CAPS affects only 0.8% of APS patients, but when it occurs it is has a mortality rate of approximately 50%.
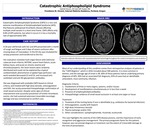
CASE REPORT: A 50 year old female with SLE and APS presented with 1 month of cough and fatigue and 2 days of severe confusion after missing doses of rivaroxaban. In the ED she was intubated for airway protection and transferred to the ICU. Her evaluation revealed multi-organ failure with extensive subacute brain infarcts, NSTEMI, severe heart failure, acute kidney injury, and acute on chronic anemia and thrombocytopenia. Her brain lesions were randomly distributed and could not be explained by a typical cardioemobolic phenomenon or global hypo-perfusion. Lab work revealed decreased C3 and C4, and increased anticardiolipin and anti-B2-glycoprotein antibodies. She was diagnosed with probable CAPS based on clinical criteria, and treated with high dose steroids, anticoagulation and IVIG. Her acuity prevented histopathologic confirmation of small vessel occlusion. Despite some signs of clinical improvement and successful prevention of further thrombotic events, she had sustained extensive irreversible neurologic damage and was transitioned to comfort care.
DISCUSSION: Most of our understanding of this condition comes from retrospective analyses of patients in the “CAPS Registry”, which in 2016 included about 500 patients. It is more common in women, and the average age of onset is 38. 60% of these patients had an underlying primary diagnosis of APS; 30% had an associated SLE diagnosis; 65% of cases had an identifiable antecedent, most commonly, infection. Diagnostic Criteria: 1. Involvement of three or more organs, systems, and/or tissues 2. Development of manifestations simultaneously or in less than a week 3. Presence of antiphospholipid antibodies 4. Histopathologic evidence of small vessel occlusion in at least one organ or tissue Treatment: 1. Treatment of the inciting factor if one is identifiable (e.g. antibiotics for bacterial infection) 2. Anticoagulation, usually with heparin 3. High dose intravenous steroids 4. Plasma exchange and/or IVIG 5. Other considerations: cyclophosphamide, rituximab, eculizumab This case highlights the severity of the CAPS disease process, and the importance of early recognition and aggressive management. The primary prognostic factor for this patient, however, was not prompt diagnosis or treatment, but the extent of irreversible damage at the time of presentation.
-

Ceftriaxone-Induced Immune Hemolytic Anemia from Treatment of Post-Treatment Lyme Disease Syndrome
Jillian Catral and Emily Hitchcock
INTRODUCTION: Drug-induced immune hemolytic anemia (DIIHA) is a rare though likely underreported entitythat is associated with significant morbidity and mortality. • Ceftriaxone is a commonly used antibiotics with a well-documented association with DIIHA. The mechanism is a drug-dependent antibody, immune-complex mediated reaction which can be severe, leading to organ failure, shock, and even death. • While the majority of cases are in children, a recent literature review had one-third of cases being adults, with up to 30-40% mortality in all ages. • This case describes an adult patient treated for the controversial diagnosis of post-treatment Lyme disease syndrome (PTLDS) which resulted in ceftriaxone-induced immune hemolytic anemia (CIIHA).
CASE REPORT: The patient is a 72-year-old active female from Minnesota with self-reported history of disseminated Lyme disease and Babesiosis diagnosed in the 1980s, Graves’ disease, hypertension, and fibromyalgia. • She presented with 3-4 weeks of progressive fatigue to being walker-dependent and mild cognitive impairment in setting of recently diagnosed normocytic anemia since starting 3x-weekly ceftriaxone-pulse therapy for PTLDS recommended by her PCP in California and prescribed by her local naturopathic doctor.
Evaluation: CBC: WBC 6.4, Hgb 9.4 (baseline ~14) with MCV 88, Plt 288 CMP: Total bilirubin 1.3 (from 1.8 two days prior to admission) Direct Coombs test: positive for IgG+complement, IgG Peripheral smear: spherocytes, schistocytes
Haptoglobin:
LDH: 343
Reticulocyte index: 7.37 % retic: 16.7 Absolute reticcount: 518
Ferritin 245, Fe 65 TIBC 408, %sat: 16
TSH 0.30, FT4 1.57
• Her ceftriaxone had already been discontinued 1 week prior to admission due to concern for DIIHA, which was consistent with her hospital workup. She was discharged home in fair but stable condition, and her anemia, energy, and cognition continued to improve in the weeks-months following.
DISCUSSION: This patient was determined to have a subacute immune-mediated hemolytic anemia with symptoms that correlated temporally with her ceftriaxone infusions. • DIIHA is a rare but potentially fatal entity with incidence of 1/1,000,000. Ceftriaxone (among other 2nd/3rdgeneration cephalosporins) and piperacillin, are commonly used antibiotics which have been associated with DIIHA. DIIHA has several mechanisms (see Figure 2). In the case of ceftriaxone, CIIHA is an immune complex-mediated reaction due to drug-dependent anti-ceftriaxone antibodies (acAb). • Other features found in CIIHA patients include acute renal failure, hepatitis, and DIC (see Figure 3). One study suggested an increased risk of CIIHA in patients with underlying conditions such as sickle cell disease and HIV, or previous exposure to ceftriaxone such as in this patient. • Treatment is withdrawing the offending drug and supportive measures as needed such as with blood transfusions. Some patients have been treated with plasmapheresis, corticosteroids, and IVIG. • 2016 Infectious Disease Society of America (IDSA) State Policy Primer on PTLDS: “The potential benefit of long-term use of antibiotics for the treatment of Lyme disease has been examined and found ineffective in multiple well-done clinical trials. … Long-term antibiotic therapy can cause many serious health consequences including protracted and intractable diarrhea, severe colitis, antibiotic resistance, allergic reactions, bloodstream infections and clots from intravenous catheters, and even death, without any scientifically-founded prospect of benefit.”
CONCLUSION: Early recognition of DIIHA (which can cause severe, sometimes fatal, reactions) and cessation of the causative agent is important to reduce the high morbidity and mortality associated with these patients. •The role of antibiotics in (and even the diagnosis of) PTLDS is contended. Potential for serious adverse effects such as DIIHA among others should be considered prior to initiating antibiotics for PTLDS. -

Delirium: Delirious Elders, Implementing Reduction Interventions Using Mobility
Michael Silvas, Joe Miller, and Shelley Sanders
INTRODUCTION: This quality improvement project involved hiring, training, and managing 3 Delirium Mobility Aids to implement a non-pharmacologic delirium prevention bundle package, including early mobility, on hospitalized patients age >65.
Background: Delirium affects 20-30% of older hospitalized patients [1]. Patients with delirium have double the mortality rate [3], which increases with delirium duration [4]. Delirium worsens long term cognitive functioning [9,10,11,12]. Hospital costs increase by $2,500 per patient, totaling $6,900,000,000 in Medicare expenditures [7]. A single delirium episode increases total yearly costs by ~$64,421 [2]. Research suggests the best treatment is non-pharmacologic multicomponent interventions [6], and those with most benefit include early mobility, reorientation, cognitive/sensory stimulation, and hydration [5].
Methods: A delirium prevention protocol was created addressing four main pillars. • Hydration: water placed within patient reach. • Sensory input: • window blinds opened by 9:00 am • hearing-aids and eye-glasses retrieved and utilized. • Soothing music via delirium TV channel for non-communicative patients. • Reorientation: oriented to person/place/time 3 times daily. • Mobility: 20-min walk (mobilization event) 3 times daily Work and time constraints prohibited existing health professionals (CNA, RN, MD, PT, OT) from implementing the protocol. Thus a new job position (Delirium Mobility Aid) was created to implement this protocol for all patients age >65 admitted to Medical A(28-bed medical unit). This was proposed to Providence St. Vincent Medical Foundation who awarded a $170,000 institutional grant for 12 months. The project residents reviewed applications, interviewed, and hired 3 CNA's to fill the position 12 hr/day, 7 days/week. Physical and Occupational Therapy trained the aids for 3 weeks in delirium management and mobilization techniques. Data was collected in Epic flowsheetsand chart notes. Confusion-Assessment-Method (CAM) is a established delirium scoring system utilized on Medical A. Data from intervention year (2019) was compared to baseline data collected 2 years prior (2017, 2018) on the same hospital unit.
Results: Preliminary data collected at month 9 of 12: • No statistically significant change in total delirium burden. However there is a trend toward decreased delirium in prolonged hospitalization (measured after day 4). For these patients with LOS > 6 days, there was a 4% reduction in late-stay delirium compared to 2018 and 10% from 2017. • 7.5-13% more patients were completely delirium free after day 4 • Length of Stay (LOS): no significant change (5.5 days) • Patients admitted from home experienced a 4% increase in discharge to home (rather than care-facility) approaching near significance (p-value 0.06). • There was a trend toward reduction in hospital falls: 2017-33. 2018-29. 2019 (present)-19, projected to reach 25 by year’s end. • Press-Ganey patient satisfaction scores remained stable.
Conclusion: Non-pharmacologic multicomponent prevention protocols, which include mobilization, implemented by specialized CNA’s, are a potentially viable treatment of delirium in elderly patients with prolonged hospitalization. This may increase rate of discharge to home, without worsening falls, LOS, or patient experience, and has a cost-savings benefit.
-
Lemierre’s Syndrome
Jennifer Nguyen and Tom Chau
INTRODUCTION: Lemierre’ssyndrome is a rare and potentially fatal complication of acute pharyngitis most commonly seen in healthy, young adults who present with neck pain and persistent, high-grade fever. It is caused by anaerobic gram-negative organisms, most often Fusobacteriumnecrophorum, spreading into the deep spaces of the neck. This leads to septic thrombophlebitis of the internal jugular vein (IJ) with septic emboli, most frequently to the lungs.
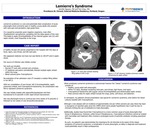
CASE REPORT: A healthy 18-year-old woman presented to the hospital with five days of fever, rigors, sore throat, and left neck pain. She appeared relatively non-toxic but was febrile to 105.6℉ and in septic shock. Her source of infection was initially unclear. Her work up included: • Normal CT neck with contrast and urinalysis. • CT abdomen and pelvis coincidentally showed multiple septic emboli within the lungs. • Blood cultures grew F.necrophorum. Re-evaluation of her admission neck CT revealed a modest filling defect in her left IJ. With her constellation of sore throat, left IJ thrombophlebitis, septic pulmonary emboli, and F.necrophorumbacteremia, her presentation was felt to represent Lemierre’ssyndrome. She was initially treated with piperacillin/tazobactamand then transitioned to IV penicillin G with rapid clinical improvement. She was discharged home to continue two more weeks of IV penicillin G followed by two weeks of oral amoxicillin/clavulanate.
DISCUSSION: What constitutes Lemierre’ssyndrome is controversial however the “classic” Lemierre’ssyndrome case consists of: • Healthy, young adult with pharyngitis. • Within 4-5 days, develops worsening neck pain, sore throat, high fevers, and rigors. • F.necrophorumbacteremia with jugular venous thrombophlebitis and disseminated septic emboli. • Most common sites for septic emboli include the lungs, joints, soft tissue, and abdomen. In retrospect, my patient’s clinical presentation was typical for Lemierre’ssyndrome, even before her blood cultures resulted with F.necrophorum. Although a rare disease with an incidence of approximately one per million persons per year, there has been a resurgence of reported cases since the 1990’s which some people hypothesize may in part be due to clinicians limiting the use of antibiotics to treat pharyngitis. Additionally, studies have found that F.necrophorumis a more common cause of acute pharyngitis than Group A Streptococcus. However, unlike Group A Streptococcus, F.necrophoruminfections cannot be treated with macrolides and treatment often involves a prolonged course of penicillin antibiotic including parenteral therapy. As such, my patient’s case demonstrates the importance for all internists to be aware of the classic symptoms of Lemierre’ssyndrome, a complication of acute pharyngitis, as delay in diagnosis and treatment could potentially result in fatal consequences.
-
Not Just Kids –A Case of Adult IgA Vasculitis
Heidi Reich and Jeff Youker
INTRODUCTION: IgA vasculitis, formerly known as HenlochSchonleinPurpura, is generally recognized as the most common form of systemic vasculitis in children, with 90% of cases occurring in the pediatric age group. However, the remaining 10% are noted in adult populations, and often has poorer long term outcomes if not identified and treated quickly. IgAVis commonly associated with streptococcal infections, although additional triggers such as drug ingestions, insect bites, and vaccinations have been described. Symptoms can include palpable purpura, acute abdominal pain, arthralgias, and hematuria. Recognizing the constellation of signs and symptoms is key for expediting appropriate therapy, which may reduce long term renal damage.
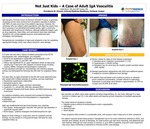
CASE REPORT: A 27-year-old man with a history of asthma presented to the ED for maculopapular rash, polyarthralgias, and myopathy. Found to be hypertensive (160s/100s) and tachycardic (115) Creatinine 1.3, ESR 13, and CRP >80 History was significant for an upper respiratory illness 10 days prior, camping trip 5 days prior with ingestion of several drugs including cocaine, MDMA, marijuana and psychogenic mushrooms. He was admitted overnight for rheumatologic and infectious disease workup, but discharged the following day with plan for outpatient follow up. Two days later, he again presented to the ED with acute abdominal pain and nausea with multiple episodes of vomiting, and was readmitted. Persistently hypertensive (160s/100s) Worsened purpuric rash Nonpitting edema in upper and lower extremities Creatinine 1.2, normal CBC, ASO titer elevated (957) CT abdomen showed small bowel edema, and EGD/colonoscopy were inconclusive His collective symptoms were reviewed and included the following: Palpable purpura without thrombocytopenia or coagulopathy Arthralgias Abdominal pain IgAVwas hypothesized and skin/renal biopsies were obtained. Skin biopsy: “leukocytoclasticvasculitis with granular IgA deposition in superficial vascular walls” Renal biopsy: “positive mesangial immunofluorescence for IgA” Based on these findings in conjunction with his symptoms and lab findings, he was started on a long steroid taper with plan for close outpatient follow-up.
DISCUSSION: IgA vasculitis can affect many organ systems including integumentary, GI, and renal. Although it is most common in children age 5-9, it can affect adults and requires prompt recognition to facilitate appropriate therapy. The classic tetrad of symptoms includes: Palpable purpura without thrombocytopenia and/or coagulopathy Arthralgias Abdominal pain Renal disease These symptoms often present in a predictable order, with purpura noted 4 days prior to other symptoms. Our patient required careful blood pressure management due to his renal involvement (started on ACEI), and steroids were initiated. At time of discharge, his renal function and rash were improving, and abdominal pain had resolved. Although full renal recovery is common in up to 89% of patients, long term renal impairment may occur. Close monitoring is imperative to minimize further renal damage.
-
Pulmonary Nocardiosisin an ImmunocompetentHost
Leah Grant, Laura Loertscher, and Jennifer Marfori
Introduction: • Nocardia is known to cause severe pulmonary or disseminated infection in immunocompromised patients, but can cause infection in immunocompetent patients. Providers should consider Nocardiosis in immunocompetent patients with prolonged and unexplained respiratory failure. • The preferred therapy for pulmonary Nocardiosis is a sulfa antibiotic for 3-6 months. Toxicity from prolonged use of alternative agents presents a therapeutic challenge in those with sulfa allergy.
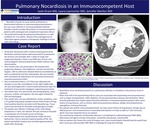
Case Report: • An 85 year-old woman with a history of paroxysmal atrial fibrillation and heart failure with preserved EF presented to her primary care provider with 1 week of cough and progressive dyspnea. Chest x-ray (CXR) was normal, and echocardiogram demonstrated known HFpEFwithout new abnormalities. • Two months later, she presented to the hospital with progressive dyspnea, chest tightness, and was found to be hypoxic. CXR on admission showed bilateral consolidations as well as mediastinal and hilar adenopathy. She was treated with ceftriaxone & azithromycin for presumed community-acquired pneumonia (CAP). • Due to treatment failure, a CT Chest was obtained and showed a mass-like consolidation in the right middle lobe; she was discharged with a several-week prednisone taper for treatment of presumed cryptogenic organizing pneumonia. • Two weeks later, she returned for worsening dyspnea, chest pressure, malaise, and hypoxia. She was again treated for CAP and discharged. • One month later, she was admitted for similar symptoms, and a CT-guided lung biopsy showed several small clusters of long Gram-positive bacteria consistent with Nocardia spp. Tissue culture was positive for Nocardia cyriacigeorgicacomplex. • The patient was offered a challenge of her sulfa allergy (reported as a rash), but refused. She was started on linezolid in anticipation of a 6 month course of therapy. • Her hospitalization was complicated by cardiac & renal dysfunction. Due to severely impaired quality of life, the patient elected for hospice care and died approximately 2 weeks after discharge.
Discussion: • Nocardiosis most commonly presents as a pulmonary infection as inhalation is the primary route of exposure. • More than half of all reported Nocardiosis cases are associated with preexisting immunocompromise such as organ transplantation, AIDS, diabetes, chronic granulomatous disease and alcoholism. More recently published case reports depict Nocardia infections in immunocompetent patients with a prior history of lung disease, such as chronic obstructive pulmonary disease, allergic bronchopulmonary aspergillosis, and bronchiectasis. • Our patient was neither immunocompromised, nor had a prior history of lung disease, though was an elderly person. Immunosenescenceis associated with decline in innate as well as T-cell immunity, which may have imparted risk to our patient. • The mainstay for treatment of Nocardia infections is trimethoprim-sulfamethoxazole (TMP-SMX). Alternative oral agents include minocycline, amoxicillin-clavulanate, and linezolid. • Had our patient not chosen the route of hospice care, close monitoring for linezolid toxicity would have been necessary with possible TMP-SMX re-challenge for long term therapy.
-
Purpura fulminans due to MSSA Toxic Shock Syndrome
Leah Grant and Rachel Plotinsky
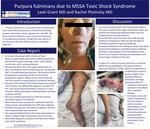
Introduction: Purpurafulminansis a rare and serious complication of anacute infectious process, characterized by large purpuricskin lesions, fever, hypotension, and DIC. The mostcommon infectious cause of purpurafulminansismeningococcal disease, though few case reports in theliterature describe Staph aureusas a causative organism.
Case Report: •A 53 year-old woman with a history of heart blocks/ppacemaker placement in 2002 presented to the ED withnausea, vomiting, fevers, chills, diffuse muscle pain and asyncopalepisode. •She was found to have multi-organ dysfunction on labs,including AKI and thrombocytopenia.On hospital day 2, shedeveloped acrocyanosis. She became febrile & hypotensive requiring transfer tothe ICU for vasopressor support. Blood cultures were obtained. She wasstarted on broad-spectrum antibiotictherapy . •Because of the patient’s thrombocytopenia and overall critical illness,the differential diagnosis included TTP, DIC, HUS, drug-induced hemolytic anemia, or a rare disorder calledcatastrophic antiphospholipidantibody syndrome (CAPS). •She was treated empirically for CAPS with plasma exchange,heparin, andsteroids. •Blood cultures were positive for methicillin-sensitive Staphaureus, and antibodies for CAPS were negative. •Antibiotictherapy was narrowed toCefazolin, and her infected pacemaker was extracted. •She required bilateral below-the-knee amputations as well as multiple finger amputations duetonecrosis. •Most likely diagnosis is purpurafulminansfrom MSSA toxicshock syndrome.
Discussion: • In acutely ill patients with skin findings described in this case as well as multi-organ dysfunction, there are several life-threatening diagnoses which must be recognized and treated promptly . •Given the 50% risk of mortality even with prompt initiation of therapy for CAPS, we did not delay in starting this patient on plasma exchange . •In purpurafulminans, the clotting cascade is disrupted by bacterial endotoxins and inflammatory cytokines, leading to a procoagulantand anticoagulant state, which in turn leads to intravascular thrombosis and hemorrhagic infarction of the skin . • A report of 5 cases of purpurafulminanscaused by MSSA TSS was published in the journal Clinical Infectious Diseases in 2005, and the isolated strains of MSSA were noted to produce higher-than-expected levels of endotoxins normally associated with TSS. •Treatment of purpurafulminansfrom MSSA TSS is antibiotic therapy. •It remains a rare and serious complication of acute infection which providers should keep on their differential of life-threatening illnesses associated with thrombocytopenia and purpuricskin lesions.
-

Struck By Lightning Twice
Bao-Ngoc Nguyen and Emily Hitchcock
INTRODUCTION: ANCA-associated vasculitides (AAV) refer to a group of disorders causing inflammation of small vessels which include granulomatosis with polyangiitis (GPA), microscopic polyangiitis (MPA), and eosinophilic granulomatosis with polyangiitis (EGPA, Churg-Strauss). Here I present a case of MPA vasculitis in a patient with alpha-1-antitrypsin (AAT) deficiency, and describe a proposed causal link between these two rare disease processes.
CASE REPORT: • 43-year-old man with history of newly-diagnosed AAT deficiency liver disease. • Chief complaint of subacute shortness of breath associated with hemoptysis and fever for 5 months. • Symptoms had been progressively worsening despite multiple courses of antibiotics and inhalers. • Pulmonary CT angiogram (CTPA) was negative for pulmonary embolism but showed “multifocal pulmonary infiltrates for whichpneumonia andseptic emboli could not be excluded”. • Infectious workup negative. • Positive myeloperoxidase (MPO) antibodies and findings on thoracoscopic lung biopsy most consistent with MPA. • Managed with steroids and rituximab.
DISCUSSION: • AAT is an acute-phase protein that inhibits the serine proteases of inflammatory cells, including proteinase 3 (PR3), to protect tissues from damage. •Mutations in the AAT-encoding gene SERPINA1 result in a structural change in AAT that inhibits its release into the bloodstream, leading to higher levels of proteases in the blood that can then cause excessive tissue damage. •Because increased levels of PR3 is a major component in the pathogenesis of ANCA vasculitis, a causal link between AAT deficiency and ANCA vasculitis has been proposed. There are many case reports describing this association, but the level of detail is variable based on the tests available at the time of the report. •Even though ANCA vasculitis is relatively rare, it is worth considering and pushed closer to the top of the differential list when a concurrent history of AAT deficiency is present.
-

Swimming Through Lake Placid: A Major Headache
Elizabeth Severson and Claudia Leonard
Introduction: Leptospirosis is caused by Leptospira species, a spirochete bacterium that affects animals and humans. The disease can range from mild flu-like illness to multi-organ failure. While likely underreported, the incidence according to the World Health Organization can range from 0.1 to 10 per 100,000 depending on climate Leptospirosis is commonly associated with occupational or recreational exposures
Case Report: A 43 year-old previously healthy man presented with two weeks of myalgias, fevers, neck pain and throbbing headache. The patient competed in an Iron Man event in upstate New York one month prior to presentation. Initial investigation demonstrated a mild anemia, elevated aminotransferases and negative head CT. Lumbar puncture revealed a cerebrospinal fluid (CSF) pleocytosis, normal glucose, mildly elevated protein, and negative gram stain, consistent with aseptic meningitis. The patient was started on acyclovir. Given his recreational risk factor for Leptospirosis in the setting of characteristic clinical features, we added doxycycline on admission Acyclovir was discontinued after negative HSV PCR. Within 24 hours, he improved significantly and was discharged with a course of doxycycline. Subsequently, all elements of the infectious evaluation returned negative except a positive Leptospirosis Ab. The patient’s symptoms and transaminitis fully resolved.
Discussion: Leptospirosis is among the most common zoonotic infections worldwide, however in the United States only about 100-150 cases are reported annually, mostly in Hawaii and Puerto Rico. The organism infects humans through contact with urine of infected rodents, dogs, and livestock or urine-contaminated environments. Patient’s commonly present with: • Fevers, myalgias, and headaches after an incubation time of 2 to 26 days • Other findings can include cough, arthralgias, nausea and vomiting, abdominal pain, and rash • About 40% of people have elevated aminotransferases, and 50-85% have aseptic meningitis • Severe cases can progress to jaundice, renal failure, pulmonary hemorrhage, myocarditis, rhabdomyolysis, and ARDS Leptospirosis is associated with a variety of risk factors, including occupational exposures and recreational activities. Large outbreaks are usually associated with recent rainfall or flooding. The bacteria can invade through skin abrasions and conjunctiva, or by swallowing contaminated water. The relationship between the risk of outdoor water sports and Leptospirosis infection is well described in the literature, with outbreaks around the world, including in Illinois (1998) and Florida (2005). Coincidentally, there had been significant recent rainfall with run-off into Lake Placid, the location of this patients Iron Man competition. Our patient’s CSF analysis was consistent with aseptic meningitis, but the time course was longer than expected for viral meningitis. Although rare in the United States, clinicians should consider leptospirosis in patients with aseptic meningitis, elevated aminotransferases, and potential exposure history.
-
Unpainfully Sweet
Khoi Nguyen and Alex Schafir
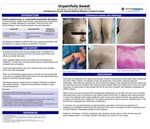
Introduction: Sweet's syndrome (ss), or acute febrile neutrophilic dermatosis, is characterized by sudden onset of fever, leukocytosis and erythematous plaques or nodules infiltrated by neutrophils. There are three main clinical settings in which Sweet's syndrome has been described: The diagnosis of Sweet’s syndrome often has a temporal association with the discovery or relapse of cancer as reported in this case.
Case Report: A 64-year-old woman with recurrent breast cancer on targeted and hormonal therapy presented to the ED with acute onset of fever and diffuse non-tender body rash. Vitals suggested sepsis and she was treated with broad spectrum antibiotics. A chest xray, viral panel, blood cultures, echocardiogram and urinalysis were unrevealing. Erythrocyte sedimentation rate and C-reactive protein were elevated. There were 90% neutrophils. When her erythematous plaques became vesicular, she was treated with IV Acyclovir for possible disseminated zoster. This was discontinued when biopsy for HSV/HZV returned negative. Skin biopsy, however, showed dense neutrophilic infiltration consistent with Sweet Syndrome. Treatment with prednisone resulted in rapid clinical improvement.
Discussion: Historically, the diagnosis of SS requires the presence of painful erythematous lesions (both Major Criteria and two of four Minor Criteria). The absence of pain and tenderness in this patient made the diagnosis challenging. After extensive evaluation to rule out infectious etiology, it was revealed through skin biopsy that her syndrome was more consistent with Sweet Syndrome despite having non-tender lesions. Given her recent recurrence of breast cancer, it was thought that her SS was more consistent with Malignancy-Associated SS (MASS) subtype. MASS is most commonly associated with hematological malignancies such as AML, but also occurs coincident with solid tumors, such as carcinomas of GU organs, breast, and GI tract. In patients with a previous history of cancer, the diagnosis of SS usually heralds the onset of recurrence. Sweet syndrome may precede, follow, or appear concurrently with a malignancy. This patient was found to have a recurrence of breast cancer in the form of bone metastases two months prior to admission. In summary, this case demonstrates an atypical painless presentation of SS and how evaluation for malignancy is indicated for patients with SS, particularly when there is an absence of other explanations such as recent infection, inflammatory disease or drug exposure. Treatment : Prednisone 0.5mg to 1mg/kgper day. Symptoms usually improve within 48 hours and skin lesions resolves within 1 to 2 weeks. Steroid is then taper over course of 4 to 6 weeks.
Providence St. Vincent Internal Medicine Residency in Portland, Oregon, stands out for its superior internal medicine training, allowing our graduates to excel in outpatient, inpatient and/or subspecialty settings. This is a collaborative, supportive and academically rigorous environment with physicians committed to patient-focused compassionate care. Our curriculum and philosophy strive to create leaders with the tools to improve the lives of their patients, as well as shaping the healthcare system of the future, their practice and their communities.
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.




